
News
A Life of Study
Clinical research co-ordinator revels in the successes, rues the
deadlines By Jean Edwards Stacey The Telegram
Karen White doesn't have time for leisurely lunches in her job as research co-ordinator for Nexus Clinical Research in St. John's.
A nurse who trained at Western Memorial Hospital in Corner Brook, where she grew up, White's work day is spent seeing patients in the morning and doing administrative work in the afternoon. Her patients are men and women participating in research studies on new drugs for treating arthritic diseases.
White describes her job as research co-ordinator as exciting and interesting.
"The best part of my job is the reward from seeing something work and work fast. The worst part is meeting deadlines," she said.
"My job comes with a huge amount of stress and independence but I don't regret working in this area. Your skills at organizing and prioritizing become highly tuned. You become a great independent decision-maker, and at the end of the day you don't pass your work over to anyone else. Your study is your responsibility and we're so busy we don't bother with long lunch breaks."
She works Monday to Friday, 9 to 5 or 8 to 4.
For the past decade, she's worked with Dr. Majed Khraishi, one of the province's five rheumatologists. Physicians who specialize in diagnosing and treating arthritis and other disorders of the joints, muscles and bones, many rheumatologists also conduct research to determine causes and better treatment for these disabling and sometimes fatal diseases.
At Nexus, there are about 20 clinical studies underway having to do with rheumatology and another 30 or so related to dermatology.
The staff includes Khraishi and White and four other full-time nurses, one part-time nurse, two research assistants, an office manager, two dermatologists and three general practitioners.
On the day we visited, White started out seeing a 32-year-old woman who was diagnosed with rheumatoid arthritis two years ago. Her disease began with swelling in one finger, spread to her hands, wrists and shoulders, lasted for months, and was so bad she could barely get out of bed.
The woman is in Week 24 of a five-year study of patients who were diagnosed with rheumatoid arthritis in the past three years, have elevated levels of inflammation, and are receiving drug therapy to see if their disease can be driven into remission. Visits are every four weeks in the first year and then every three months.
It is a blind study where there's the possibility of three different treatments: the study drug and methotrexate, the current gold standard for patients who have moderate to severe rheumatoid arthritis with pain, stiffness, swelling and fatigue; methotrexate alone in higher or lower doses; or the study drug alone.
White checks the patient's vital signs - temperature, blood pressure, pulse rate - takes blood samples, and is joined by a second nurse to carry out a joint assessment, examining 66 body joints from the top of the patient's head to her feet, and checking for tenderness and swelling.
"So, how much morning stiffness are you having now?" asks White.
"Twenty minutes in the morning," replies the patient. "And I feel it mostly in my hands."
White notes that when the patient started the study she had 28 tender joints and nine swollen joints.
Today, she's showing improvement, with five tender joints and nine swollen ones.
The patient fills out a health assessment questionnaire, providing her own assessment of her pain and how she's doing in her daily life. She ranks herself in the 20th percentile, well down from the 50th percentile mark she started with.
Khraishi comes in to ask the woman if she's having any problems, such as side-effects with the drugs, or fever. He also does a physical assessment.
White uses an interactive voice response system to call the drug company for whom the study is being done and to find out what medication to give the patient.
She enters her PIN number, presses the number for the study, enters the subject's number, enters the PIN again to ensure the patient's new supply of medication and the voice on the phone tells her what medication has been assigned, letting her know by bottle number only. The medication is then brought to the patient, who injects herself in the stomach as she was taught by White.
Participants in clinical trials receive free medication from the drug companies that commission the studies. Drug companies such as Bristol Myers Squibb, Merck Frost and Pfizer monitor studies on a monthly basis, reporting any ill-effects to a Health Canada Ethics Commission.
"This is all completely voluntary and the patient's safety is paramount," says White.
"If we felt the patient was not doing well or worsening we wouldn't hesitate to pull them from the study. The hope is that when the study is finished the patient will be in remission or that the new drugs will be readily available."
White follows up with a joint assessment on a woman from the west coast who was diagnosed with rheumatoid arthritis in 1978 and has failed previous drug therapies.
She's now in Week 12 of a five-year clinical trial and seems to be doing well. She says you can't let rheumatoid arthritis rule your life.
The next patient is a woman from central Newfoundland who was diagnosed with rheumatoid arthritis 16 years ago, at age 28. She's in Week 16 of a five-year study and appears to be doing well.
White says she remembers the woman coming in hardly able to walk and with feet so swollen she was wearing sneakers three times her usual size. Two weeks after starting new drug therapy, she was able to slip on sandals she hadn't worn for years.
At noon, White sees a 46-year-old man with rheumatoid arthritis in every joint except his hips. He's in Year 4 of a five-year study in which he is given an intravenous infusion every 28 days.
He said he's improved considerably from five years ago when he was so bad he couldn't turn the ignition key in his car or lift anything heavier than 10 pounds.
White checks his vital signs before hooking him up to the IV machine and smiles as he says they've become like brother and sister. His infusion takes 30 minutes; some take as long as five hours.
The drug he takes is being marketed, but White's previous patients are taking drugs that are not yet on the market.
In the afternoon, White is busy processing blood and doing office work. All patient information goes into a computer for entry into a central database.
In the studies she's currently involved in, all blood is shipped to a central laboratory in the U.S., with reports back within 48 hours.
There are 5,000 diagnosed rheumatoid arthritis patients in this province, most in their 40s and 50s.
White speaks of her patients with admiration.
"Rheumatoid arthritis patients are a very nice group of people," she said.
"They're a unique group of people who have a debilitating disease but a great outlook. For the most part, they tend not to give in to their illness. The rewarding thing for us in the past few years is seeing how fast these biologicals work."
Biologicals are medical preparations made from living organisms or their products for use in diagnosing, immunizing or treating animals or humans, or in related research.
Introducing ...
Name: Karen White
Age: 50
Job title: Clinical researcher
Years on the job: 12
Hometown: Corner Brook
What was your first job? Waitress in a restaurant when I
was in high school. If you could choose any other profession, what would it be?
Even when I was a young girl I can't remember even suggesting I would be
anything else but a nurse.
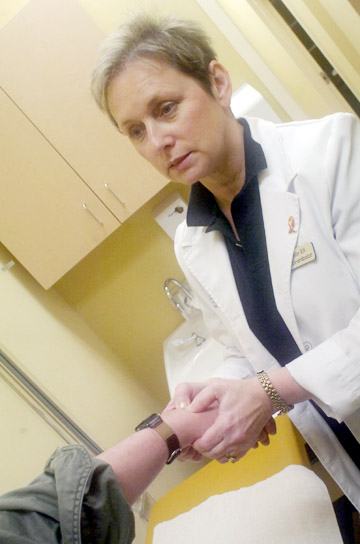
Karen White Research co-ordinator
Karen White examines a patient at the Nexus Clinical Research in St. John's.
- Photo by Keith Gosse/The Telegram
